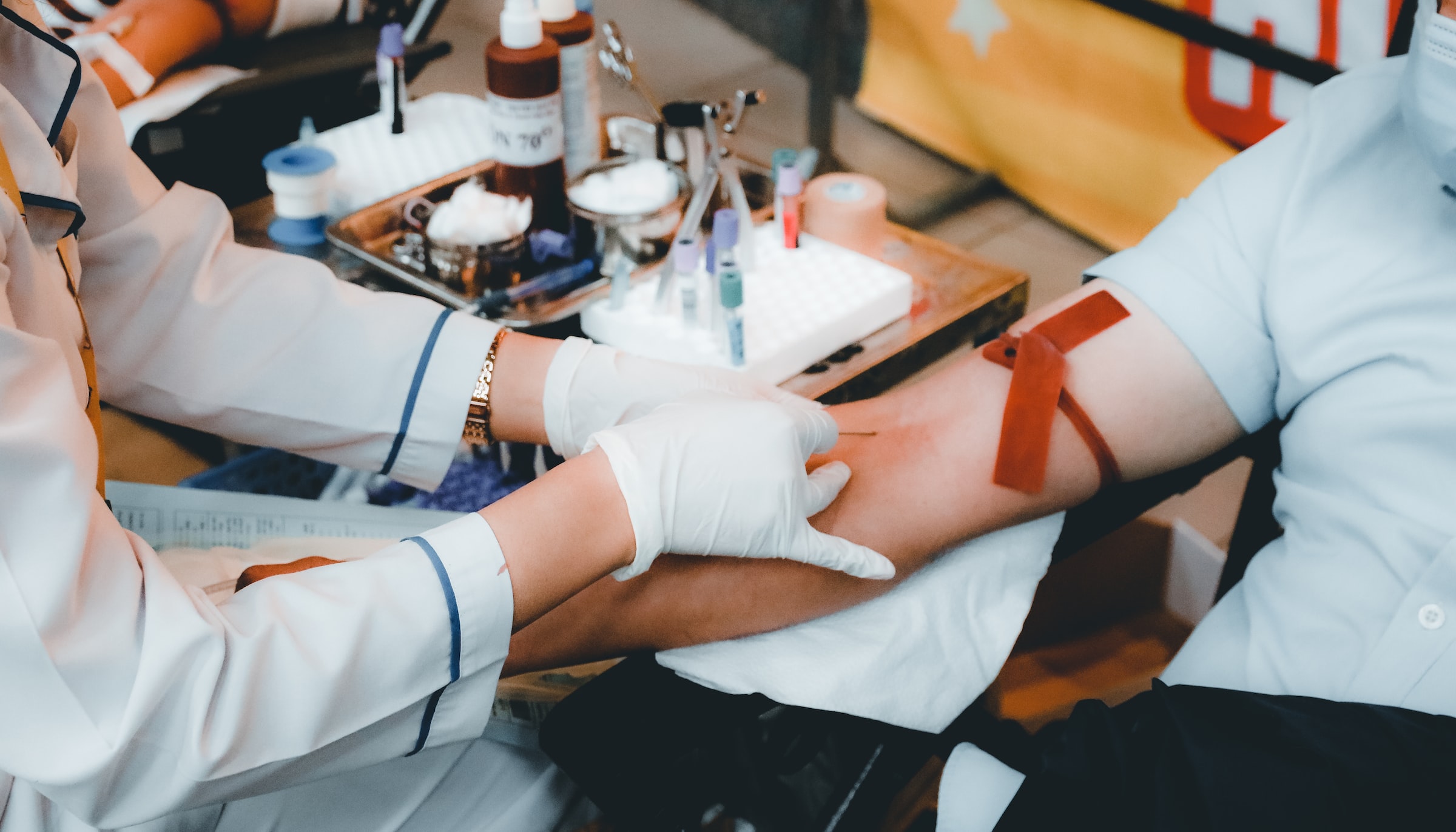
Medical Laws All Doctors Should Know
Most doctors are not attorneys. But that doesn't imply they have to be completely ignorant of the medical laws.
Author:K. N.Nov 26, 20221.9K Shares491K Views
Most doctors are not attorneys. But that doesn't imply they have to be completely ignorant of the medical laws.
Medical Laws
The practice of medicine is increasingly impacted by the law as a result of intense public scrutiny. LNN and Stationzilla, a legal website and a medically certified website, have come to our assistance with this essay that is non-technical, easy-flowing, and non-taxing to the brain yet totally relevant.
Busy medical professionals cannot cope with textbooks full of legal jargon.
HCQIA Law
The rise in medical misconduct led to a reduction in healthcare quality, which gave rise to the Health Care Quality and Improvement Act of 1986 (HCQIA). At the time, unqualified doctors were changing states without disclosing their previous unqualified performances.
Physicians were unjustly deterred from actively participating in professional peer review by the possibility of financial penalties. Physicians who take part in the peer evaluation of potentially incompetent physicians are protected from financial harm under the HCQIA of 1986 (HCQIA).
At the time, unqualified doctors were changing states without disclosing their previous unqualified performances. Physicians were unjustly deterred from actively participating in professional peer review by the possibility of financial penalties. Physicians who take part in the peer evaluation of potentially incompetent physicians are protected from financial harm under the HCQIA.
Additionally, the HCQIA established procedural guidelines for due process, privilege constraints, reporting, and information dissemination, in addition to creating a national practitioner data bank to track ineffective, incompetent, or unprofessional doctors.
CHIP Law
Children in families that make too much money to be eligible for Medicaid can get access to inexpensive health insurance through the Children's Health Insurance Program (CHIP), a cooperation between the federal and state governments.
Pregnant women are also covered under CHIP in several states. Each state closely coordinates its Medicaid programwith the CHIP coverage it provides.
State-specific CHIP benefits differ, but all offer children complete coverage, which covers regular checkups, vaccinations, office visits, and prescription drugs. It's significant to note that each state program has its own unique requirements for CHIP eligibility.
Take Action Against Kickbacks
Receiving compensation for referrals when participating in federal healthcare programs like Medicare and Medicaid is prohibited by the Anti-Kickback Act of 1986.
Payments for referrals can include cash, free rent, vacation, food, or exorbitant fees for consulting or medical directorships. Referrals can be for medications, supplies, or healthcare services. A few exclusions, referred to as "voluntary safe harbors," have been enacted into law.
Being a source of referrals for other doctors or other healthcare suppliers and providers makes you a desirable target for kickback schemes. According to the HHS, "you select what medications your patients consume, which doctors they see, and what healthcare services and supplies they receive."
HRRP Medicare Law
The Hospital Readmissions Reduction Program (HRRP), a Medicare value-based purchasing program, reduces payments to hospitals that unnecessarily readmit patients. It is a component of the Affordable Care Act. The program's goal is to link hospital care quality and funding.
PSQIA Act
A voluntary reporting system is established under the Patient Safety and Quality Improvement Act (PSQIA) of 2005 in order to enhance the data that can be used to identify and address patient safety and healthcare quality problems.
In order to achieve this, the PSQIA offers patient safety information federal privilege and confidentiality protections.
For breaches of patient safety and confidentiality, HHS may impose civil monetary penalties under the PSQIA.
In addition, the PSQIA gives the Agency for Healthcare Researchand Quality permission to monitor patient safety organizations, which are teams of outside specialists who gather and analyze data on patient safety.
EMTALA Labor Act
It is difficult to imagine a world without the Emergency Medical Treatment and Active Labor Act (EMTALA), which was passed in 1986.
By compelling healthcare professionals to give medical care regardless of the patient's capacity to pay, this law ensures access to emergency healthcare.
When a patient is injured or giving birth, for example, the law mandates that caregivers stabilize the patient and continue treating them until the patient is stable. If the care provider is unable or unwilling to do what the patient needs, the patient must be moved to another facility.
Stark Law
A doctor is prohibited from suggesting patients receive Medicare or Medicaid treatments in which the doctor has a financial interest under the Physician Self-Referral Law, also known as the Stark Law.
For instance, it is probably against the Stark statute for a doctor to refer a patient to their own home health company. The legislation does, however, permit a few exceptions.
So long as there is no possibility of financial exploitation, a group practice might be permitted to refer patients for in-office auxiliary services like lab testing or radiology imaging.
GINA Federal Law
The Genetic Information Nondiscrimination Act (GINA), established by the federal government, prohibits employers and insurance providers from treating people unfairly based on the results of genetic testing, such as a test for the sickle cell illness that affects African-Americans.
Genetic information cannot be used by employers to decide who gets hired, fired, promoted, paid, or given a certain job.
The same rule applies to the use of genetic data by health insurers in determining eligibility, coverage, underwriting, or premium rates. Employers and insurance companies are not allowed to make job applicants take genetic tests before being hired.
HITECH Act
In order to encourage the use of health information technology among healthcare professionals, the Health Information Technology for Economic and Clinical Health (HITECH) Act was passed into law in 2009.
The privacy and security of electronic transmission of health information are covered in part under the HITECH Act. Additionally, it increases HIPAA regulations' civil and criminal enforcement.
This law establishes four levels of culpability, with the lowest-level violators being given the chance to make amends.
False Claims Act
In reaction to fraud by dishonest contractors who were defrauding the US military, the False Claims Act was passed during the Civil War. This law is well known today for holding people and organizations accountable for defrauding government programs like Medicare and Medicaid.
Upcoding for medical procedures and conducting or ordering superfluous procedures are common legal breaches. A legal clause known as the "qui tam provision" makes it easier for people to file lawsuits on behalf of the government and promotes whistleblowing.
People Also Ask
What Are Examples Of Medical Ethics?
- Patient Privacy and Confidentiality.
- Transmission of Diseases.
- Relationships.
- End-of-Life Issues.
- Ethical Issues in Healthcare in an Online MBA Program.
What Is The Medical Ethics?
Medical ethics is concerned with the duties that doctors, hospitals, and other healthcare providers have to patients, society, and other health professionals.
The health field has a set of rules about what is right and wrong that apply to all health workers and medical facilities.
What Is Common Law In Medicine?
This means that a doctor can't share private information unless there's a good reason to do so under the law.
Conclusion
Even if a certain rule, like the Stark Law, does not pertain to your line of work, it is still necessary to be aware of it. You can report illegal activity if you witness it, potentially protecting yourself, your institution, and your patients from responsibility and harm.

K. N.
Author
Latest Articles
Popular Articles